SECTION 1. RATIONALE FOR STAKEHOLDER AND COMMUNITY ENGAGEMENT IN QUALITY IMPROVEMENT INITIATIVES
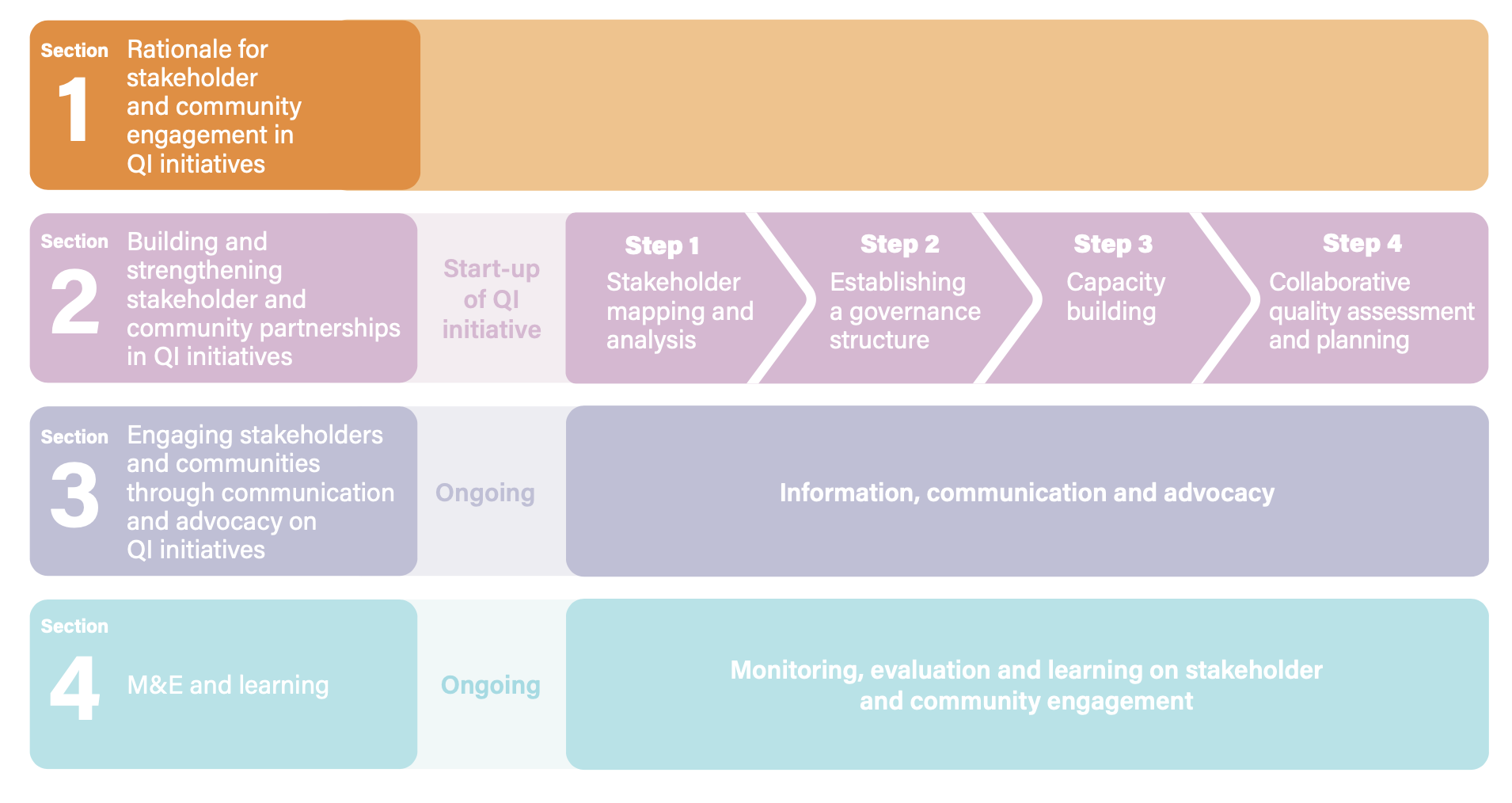
While QoC is predominantly expressed at the level of the interaction between health providers and service users, it takes place within a much broader context, including the larger health system. At each level of the health system and in the different steps of the QI process, stakeholder and community engagement is crucial and will be shaped according to national, district and facility strategies to improve QoC. The rationale for engaging stakeholders and communities is generally perceived as follows:
-
Inclusion of broader determinants and intersectoral collaboration in QI initiatives. QoC is a product of the wider health system and of social, political and economic determinants. The underlying causes of problems and the opportunities for solutions will be found across different disciplines and across the workings of government, private sector and civil society. By including stakeholders from different disciplines and sectors (e.g. water and sanitation, education, social affairs, finance, transport, local development), the complexity of factors that influence QoC in MNCH will be better understood. For example, as a key component of safe and quality services, water, sanitation and hygiene (WASH) improves not only health outcomes and the experience of care, but also staff morale and the efficiency of services. (14)
-
Contribution of different stakeholders. Although health system actors (MOH, decentralized departments, programmes and facilities) may lead the QI initiative, it is dependent on a range of stakeholders for successful implementation, including from those who influence factors beyond the direct provision of care, and those who have a direct or indirect influence on funding, resources and provision of services. These different stakeholders will need to contribute to the development of QoC plans, their implementation, and M&E.
-
Institutionalization of quality. Through sustained stakeholder and community engagement, a culture of quality can be fostered whereby QoC in MNCH is advocated for and prioritized in policy and programming across the health system. Improving stakeholder and community engagement in QI initiatives for MNCH can also benefit other health services by putting quality on the agenda and by encouraging users to seek higher-quality services for all of their health-care needs.
-
Relevance and buy-in. In a resource-constrained environment with competing health priorities, quality of MNCH may not always be a priority. Advocacy for a focus on QoC can be challenging. It is crucial to identify and engage key decision-makers and policy influencers to make the case for investment in QoC and to create an enabling and supportive environment for QI initiatives, including through increased support for stakeholder and community engagement. (15) By including a range of stakeholders, plans are better tailored to local contexts and to implementers’ and users’ realities. Plans have more potential to harness buy-in. Leaving out key groups or involving them too late in the process can undermine efforts to create effective partnerships.
-
Learning and promoting synergies. Many countries are implementing multiple QI initiatives in MNCH and other sub-sectors. Stakeholder and community engagement allows for the opportunity to coordinate efforts and to share experiences and lessons learned across initiatives, in-country, between districts, and as well as cross-country. (16) Districts constitute important platforms for in-country learning by bringing together different stakeholders, encouraging their participation and contribution, strengthening synergy and avoiding duplication. Stakeholder engagement at the district level allows for the opportunity to share lessons across initiatives, not only with different health facilities but also with community representatives, local authorities, nongovernmental organizations (NGOs), and between districts.
-
The right to participation and empowerment. Women’s right to health and their right to participate in public life and political decision-making is enshrined in international legal frameworks such as the Committee on the Elimination of Discrimination Against Women (CEDAW) and the Protocol to the African Charter on Human and Peoples’ Rights on the Rights of Women in Africa – better known as the Maputo Protocol. The latter provides for the protection and promotion of women’s reproductive health rights, their dignity and non- discrimination in service delivery. The effective implementation of this right involves providing women and vulnerable groups opportunities to gain enhanced skills, knowledge and confidence to play an active role in QI initiatives and to participate in designing and implementing national health policies and programmes.
-
Enhancing accountability. Accountability is both a mechanism and a process by which government, service providers, private actors, community members and other stakeholders are required to demonstrate, explain and justify how they have fulfilled their obligations towards quality MNCH. (17) Having mechanisms for the inclusion of users’ voices during development of the strategy is important, but their voices are equally important when it comes to implementing and monitoring the strategy and ensuring accountability against jointly defined goals, targets and outcomes. (18) Stakeholder and community engagement can ensure that governments, health providers and other stakeholders are held accountable for decision-making and for the services and quality they provide. (19)
-
Enhancing accessible, acceptable, respectful and people-centred MNCH care. This kind of care can be enhanced through the integration of users’ and communities’ perspectives on QoC. Factors that affect the uptake and outcome of care are socioeconomic and cultural characteristics, accessibility of health facilities and QoC. (20) People’s perceptions and experiences of quality – rather than clinical indicators of quality – are what drive service uptake and outcomes. Perceptions are shaped not only through individual encounters between service users and providers, but also by users’ social networks, community norms and values, and peer influences. (21) Stakeholder and community engagement can provide opportunities to better understand QoC from service users’ and communities’ perspectives and to develop context-relevant QI initiatives that integrate social norms of acceptability and quality across the continuum of MNCH care.
-
Stakeholder and community ownership. Stakeholder and community engagement can enhance communities’ awareness of QoC, conditions of QoC and health systems challenges and scarcities; clarify expectations; and strengthen the communities’ role in contributing to creating an enabling environment for QoC. Reorienting care around the needs, preferences and engagement of users and communities by health providers can be a powerful step to institutionalize QoC and increase the lifespan of QI activities. (22)
The link between stakeholder and community engagement and QoC improvement has not always been explicit. QoC has often been considered the professional domain of health planners, managers and health providers. While community engagement and participation have often been translated to community involvement in health promotion and programme implementation – or in some programmes, limited to introducing community health workers – it has been under-developed in QI initiatives. (23) “Communities” were mainly seen as passive recipients or beneficiaries of services and less as “stakeholders” with interests, influence and relevant contributions in areas to improve planning and service delivery, including in QI and monitoring. Community engagement as a QI strategy has recently emerged in the form of community-based monitoring interventions, or the introduction of client feedback mechanisms, also in MNCH. (24) A survey conducted in 2018 by WHO found that 60% of countries in the WHO regions (ranging from 47.1% in the Western Pacific to 72.7% in South-East Asia) have mechanisms in place at the facility level to solicit feedback on quality and access from community members, users and families. (25) Though linkages are emerging, the integration of stakeholder and community engagement in QI initiatives in a systematic and meaningful way, rather than only as a stand-alone QI intervention, remains a challenge in many settings.







 Next Chapter
Next Chapter